Sarah's Pharmaceutical Story—Part 1
Sarah is an active, energetic, and basically healthy 85-year-old woman.
Many years ago, her physician prescribed meds to her based on the "one-size-fits-all" practice common in that era. Back then, the medical community knew little about the impact neurotransmitters had on the overall mental wellness of an individual.
Doctors would ask a few questions, might take a couple of random tests, and hand out a prescription to help deal with the symptoms of fatigue, anxiety, and other mental conditions as well as physical pain. Treating the symptoms, not the cause, was the standard practice twenty years ago for physical symptoms caused by brain & body chemistry conditions—there just was not a lot of medical knowledge on hormones and neurotransmitters back then.
She had continued taking the meds, despite struggling with the symptoms and side effects. Recently, Sarah felt ready to get an updated perspective of her underlying condition. She was curious as to whether there were more current alternatives to all the meds. She chose to have her neurotransmitters tested.
Sarah's Choice to Test Her Neurotransmitters
* The comments below are for information purposes only and are not to be construed as medical advice. These suggestions are not intended to diagnose, treat, cure, or prevent any disease. Comments are related to a specific individual and may have completely different results from your own. Please consult your healthcare practitioner for diagnosis and treatment.
Sarah is socially engaged with her neighbors, a leader in her religious community, an avid gardener, and lives a full life.
Seventeen years ago she began seeing a psychotherapist for her mental health and a physician for her medical conditions. She suffers from arthritis pain and severe insomnia, struggles with poor memory, and vacillates between anxiety and depression.
Her physician has Sarah taking Trazodone, an SSRI for sleep; Clonazepam, a benzo for anxiety; 2 g of a GABA supplement for anxiety; acetaminophen (analgesic) and ibuprofen (NSAID) for her arthritis pain; and a melatonin supplement for sleep. She wondered if there were a better alternative to the ongoing daily consumption of the benzodiazepine, analgesic, and NSAID.
In 2021, Sarah decided to try something different.
She was tired of taking pharmaceuticals. She spoke with her long-time psychotherapist and expressed her desire to find a healthier alternative to all the pharmaceuticals. He was aware of the rapid advances in lab testing and the results provided, giving a clear picture specific to the individual. Conventionally trained doctors can't keep up with the variety of lab tests that detect hormone and neurotransmitter imbalances, and he believed that they could find a more natural solution. The neurotransmitter test chosen was able to highlight the areas most likely to be the source of anxiety, depression, insomnia, and poor memory.
The neurotransmitter test selected measures the levels of
- Two primary inhibitory neurotransmitters: GABA and serotonin
- Five primary excitatory neurotransmitters are dopamine, norepinephrine, epinephrine, glutamate, and PEA
- Report the ratio of norepinephrine to epinephrine
- Level of creatine
- And two primary adrenal hormones, cortisol (x4) and DHEA-S (x2), were sampled throughout the 24-hour day.
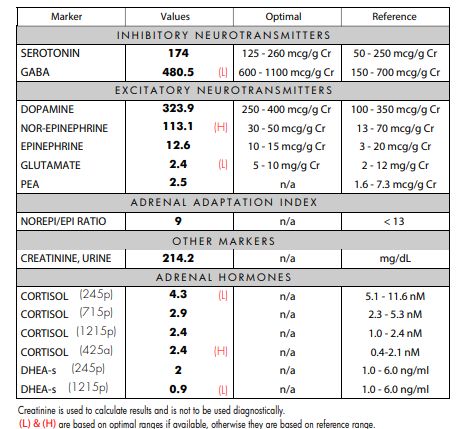
Neurotransmitter Test Results
Sarah and her therapist weren’t surprised by the neurotransmitter lab report.
There were three neurotransmitters and three hormone levels that were out of the optimal range—each directly correlating to her symptoms.
INHIBITORY VS. EXCITATORY NEUROTRANSMITTERS
Keeping the inhibitory NTs and excitatory NTs in balance with one another is essential in avoiding anxiety, depression, fatigue, sleep disorders, and other conditions.
Excitatory neurotransmitters are not necessarily exciting—they are the "on switch" that revs us up to get going. Those that relax brain activity and help create balance are called inhibitory.
Inhibitory NTs are the "off switch" that calms us down. Inhibitory neurotransmitters balance mood and are easily depleted when the excitatory neurotransmitters are overactive. This quick depletion is an important part of understanding the lab report.
Upon interpreting her results, the lab consultant and her therapist could see that her inhibitory neurotransmitters that controlled her sleep cycle were out of range. The lab results also indicated that some of her current treatments were likely creating issues that were preventing her from finding relief. On top of that, Sarah had three levels of stress hormones that were suboptimal, which likely contributed to both her anxiety and her insomnia.
GABA is a primary inhibitory neurotransmitter that promotes calm and manages sleep. Sarah’s GABA levels were below the optimal range, even though she was taking a very high dosage of GABA supplements, which was concerning. It was a sign of a “leaky gut,” which is an inability of our stomach to adequately absorb nutrients. It’s a common side effect of continued use of ibuprofen, which Sarah was taking for her arthritis pain. Taking excessive amounts of GABA is known to lead to symptoms of anxiety and heart racing. Her glutamate levels were also low; glutamate is the precursor to GABA.
Sarah’s norepinephrine levels were high, which was also likely a factor in her anxiety, since norepinephrine, also known as noradrenaline, is an adrenal hormone that is responsible for our body’s stress response. This imbalance is commonly caused by continued daily use of acetaminophen, which was for arthritis pain.
Cortisol is another one of our body’s major stress hormones. It fluctuates throughout the day in an ebb and flow that is called the diurnal cortisol curve. It is most commonly at its highest level in the morning when it wakes us up and at its lowest level at night, right before we go to sleep. The opposite of this norm is true for Sarah.
Her levels of the stress hormone cortisol were higher than optimal when she was preparing for sleep, which leads to insomnia and restlessness, and significantly lower than optimal after she had woken up, leaving her feeling groggy and apathetic.
Sarah had been taking an SSRI called Trazodone for sleep for years along with melatonin but was still struggling to sleep.
Sarah’s test also indicated that one of her DHEA-S levels was low. DHEA-S supports memory and hippocampus health and also has been linked to depression.
Her serotonin level was optimal but could likely be an issue that is masked by her SSRI Trazodone that she is prescribed for sleep.
Her Treatment Plan
Based on these findings, her therapist came up with a plan for Sarah to hopefully address the root of her symptoms and to be able to safely wean her off the pharmaceutical medications she was taking, with the involvement of her physician's supervision.
Her plan included
- Replacing her SSRI with a cortisol-lowering supplement called Seriphos coupled with a Melatonin supplement,
- Replacing her current Arthritis treatment of Ibuprofen and Tylenol with a glucosamine supplement called ArthroMax Advanced and considering a CBD topical salve for pain,
- Lowering her current GABA supplement by 75% to 500mg daily and adding 3 g of a Glutamine supplement,
- Adding a natural supplement called Lentra (by Sanesco) to relieve anxiety and repair suspected damage to her stomach (referred to as "leaky gut") by ibuprofen,
- Adding DHEA-S and Phosphatidylserine supplements to aid in memory,
- Beginning her day with scheduled social interaction to aid with her depression,
- And retest her levels in 6-8 weeks to track progress and get an accurate reading of her serotonin level.
Your Hormone Management Testing Plan
- Step 1: Start by selecting and ordering your desired test(s). You will receive an at-home testing kit that fits your unique concerns and needs. No prescription or visit to the doctor’s office is required. Your test kit is delivered directly to your front door.
- Step 2: Take the test to establish the starting hormone baseline at the beginning of your plan. Consider developing your plan alongside:
- a licensed health care provider for medical conditions, especially for severe "out of normal range" results
- or a Health Care Coach for nutrition and supplements that will support your desired results
- Step 3: Develop a plan based on your hormone test results, establishing a one-year or more outlook.
- Keep logs of your intakes, and daily routines related to your hormone test results.
- Keep logs of your intakes, and daily routines related to your hormone test results.
- Step 4: After 6-12 months of actively working on your plan, take the same test again to determine your progress.
ZRT Neurotransmitters Profile
 See our ZRT Neurotransmitters Profile to check your neurotransmitter levels. Samples are taken from dried urine, with the exception of the saliva steroids add-on option.
See our ZRT Neurotransmitters Profile to check your neurotransmitter levels. Samples are taken from dried urine, with the exception of the saliva steroids add-on option.
Neurotransmitters Test Kit Includes:
Neurotransmitters Dried Urine: GABA, Glu, Gly, DA, Epi, NE, HIST, 5-HT, PEA, DOPAC, HVA, 5-HIAA, NMN, VMA, Trp, Kyn, 3-OHKyn, Tau, Gln, His, N-MeHist, Tyra, KynAc, Xanth, Tyr, Crtn
Available Neurotransmitter Add-ons:
You will be able to include these add-ons during the ordering process for the Neurotransmitters Panel.
Neurotransmitters + Saliva Steroids Concerned about hormone imbalances? Use the tube in the Neurotransmitter kit to collect a Saliva sample for Estradiol, Progesterone, Testosterone, DHEA-S & AM Cortisol.
Neurotransmitters + Diurnal Cortisol (UDH) I Don't want to test Melatonin. Add only Free Cortisol & Free Cortisone x4 to the same samples being collected for Neurotransmitters.
Neurotransmitters + Diurnal Cortisol & Melatonin UDH II - For concerns about adrenal or sleep issues, add 4-point Cortisol, Cortisone & Melatonin to the same samples being collected for Neurotransmitters.
Neurotransmitters + Diurnal Cortisol, Melatonin, Norepinephrine & Epinephrine UDH III For concerns about adrenal or sleep, stress issues, add Free Cortisol x 4, Free Cortisone x 4, Melatonin (MT6s) x 4, NE x 4 & Epi x 4 to the same samples being collected for Neurotransmitters.
add 7 Toxic Heavy Metals Urine Elements – $99 – Add tests for Iodine, Bromine, Selenium, Lithium, Arsenic, Cadmium & Mercury
Additional Resources
- Neurotransmitter Fact Sheet
- Neuroendocrine Imbalances and Depression
- Our Emotions Reflect Our Neurotransmitter Hormone Balance
- Why You Might Be Starving Your Brain
- Dopamine and New Year's Resolutions
- Neurotransmitter Disruption and Adrenal Function
- Neurotransmitter Imbalances and Mood Disorders
- Forbes Article
Related Articles on Neurotransmitters
Alex's Story: Imprisoned by Neurotransmitter Imbalance (Part 1)
Alex's Story: Freed from Neurotransmitter Imbalances (Part 2)


